Research suggests that 40% of people experience benzodiazepine withdrawal if they use it for more than six months. The other 60% also suffer from mild symptoms. Benzos are only safe when used for a limited time and under clinical recommendations. Any extended usage is always accompanied by inconvenience withdrawal symptoms that require proper rehab and clinical withdrawal.
ChoicePoint Drug Rehab provides safe benzo withdrawal through Medication-assisted Treatment. Call Now 844.445.2563 to get your appointment!
Table of Contents
How Commonly Prescribed Benzodiazepines Can Pose Life-Threatening Dangers?
Benzodiazepines, commonly termed “Benzos,” are prescription drugs, mainly Sedatives. They work mainly as central nervous depressants and actively lower brain activity by binding to GABA receptors in the brain, producing calming effects.
Benzos are prescribed for treating:
- Anxiety disorders (Xanax®, Librium®®, Ativan®, Valium®)
- Seizures disorders (Klonopin®, Ativan®, Valium®)
- Insomnia (Dalmane®, Halcion®, Restoril®)
- Providing anesthesia (Ativan®, Valium®, Versed®)
- Muscle relaxation (Valium®)
- Alcohol withdrawal (Valium®, Serax®, Ativan®, Librium®®)
Prescription of benzodiazepine for alcohol withdrawal is only dispensed under DEA-certified staff of inpatient rehab to avoid concurrent withdrawal symptoms. However, some people use it for recreational purposes as well as to increase the dose to have long-lasting effects, which results in dependence and shows signs of benzo addiction.
Types of Commonly Available Benzodiazepines
Benzodiazepine is a general class of sedatives, or CNS depressants, described as schedule IV drugs in the Controlled Substance Act of DEA. These are categorized into subclasses depending on their function type:
- Alprazolam (Xanax®)
- Chlordiazepoxide (Librium®®)
- Halazepam (Paxipam®)
- Lorazepam (Ativan®)
- Oxazepam (Serax®)
- Prazepam (Centrax®)
- Quazepam (Doral®)
- Midazolam (Versed®)
- Flurazepam (Dalmane®)
- Triazolam (Halcion®)
- Temazepam (Restoril®)
Whereas, some of the anticonvulsant benzodiazepines include:
- Clonazepam (Klonopin®)
- Diazepam (Valium®)
- Clorazepate (Tranxene®)
Limited use does not cause any harm, but due to excessive prescriptions and easy availability, these drugs are often misused or used without clinical guidance, resulting in benzodiazepine addiction.
Signs and Symptoms of Benzo Dependence: Look Out for Risky Warnings
Benzodiazepine addiction and dependence come with severe withdrawal symptoms that are highly unmanageable, disturbing, and varied. Physical symptoms of benzo dependence are:
- Pains
- Muscle twitches
- Blurred vision
- Seizures
- Gastrointestinal symptoms, i.e., nausea, vomiting, constipation,
- Heart palpitations
- Sweating, skin rashes
Psychologically associated dependence on benzos shows:
- Hallucinations
- Depression
- Paranoid thinking
- Memory loss
- Poor concentration
- Aggression
- Irritability
- Social phobia
- Anxiety and panic attack
Some of the risky warnings of benzo overdose include:
- Extreme drowsiness
- Decreased reflexes
- Impaired coordination
- Coma
- Death
Combining Benzo with opioids can result in Profound sedation, Respiratory depression, and death. Seek immediate help from professionals 844.445.2563 if someone experiences any of the withdrawal symptoms to avoid fatal consequences.
Why Safe Withdrawal from Long-term Benzo Abuse Matters
Some drugs are safe to quit on your own, but benzodiazepines are the worst of all. A person using long-term withdrawal must stop immediately and go for a comprehensive withdrawal treatment because withdrawal can help avoid
- Addiction
- Central nervous system depression
- Cognitive decline
- Decreased motor functioning
- The fatal reaction of benzo combinations with alcohol, sedatives, and opioids
When benzos are removed from your system, the brain experiences a rebound because GABA and dopamine levels, which are involved in the brain’s normal functioning, decrease. Resulting in risky outcomes such as:
Reoccurring Withdrawal Symptoms
When benzodiazepines are suddenly abandoned, withdrawal symptoms previously treated or fresh will come with greater severity and can cause powerful effects, both physical and psychological. The only way to come out of this is benzodiazepine medications in detox.
Pregnancy and Benzodiazepines
Benzos, when used during pregnancy or before planning pregnancy, may interrupt the cycle and come with fetal syndromes. All forms of benzos cross the placenta and harm the fetus with:
- Floppiness (decreased muscle tone)
- Preterm birth
- Low birth weight
- Sedation
- Neonatal respiratory distress
Therefore, expert tapering can reduce such effects, but doing so alone might bear fatal consequences for the expecting mother.
Co-occurring Disorders
Individuals with underlying psychological conditions such as PTSD, Anxiety, trauma, Depression, and bipolar disorder may feel intense withdrawal due to cognitive impairment of benzodiazepine withdrawal. Such individuals require a dual diagnosis treatment to treat the side effects holistically.
Risk Factors of Benzodiazepine Withdrawal
People who are at greater risk of experiencing the worst Benzo withdrawal symptoms include those:
- suffering from co-occurring disorders
- who are alcoholic
- with age above 60
- individuals using combination sedatives or opioids
- having a history of psychiatric disorders
- using high potency, short-acting benzos
- genetic factors or history of substance use
All of these factors may aggravate the withdrawal effects of benzodiazepines.
Timeline of Benzodiazepine Withdrawal Symptoms
Benzos are intended to be taken for only a few weeks. Long-term benzo usage makes the brain and body dependent on them and causes withdrawal symptoms if not taken regularly.
Benzodiazepine withdrawal tends to appear from hours to a few days after the last use. But there are some factors to consider that affect Benzo’s stay in your system, such as:
- Type of benzo taken
- Individual’s metabolism
- Dosage and way of taking benzos
- Individual’s physical and psychological health
- Co-occurring disorder
Benzo withdraws from the body in certain phases, and every symptom appears at a given timeline.
Phases of Benzodiazepine Withdrawal
According to APATF, discontinuing benzodiazepine withdrawal is associated with three psychological events or phases such as:
A. Rebound (Early Withdrawal)
Withdrawal symptoms such as insomnia and anxiety usually begin the first 6-8 hours of benzodiazepine withdrawal and may persist for up to 4 days. Rebound anxiety and insomnia peak at 1-2 days duration.
- People who take short-acting benzos experience this phase on the first day.
- People using long-acting benzos usually face its initial symptoms on the 3-4th day.
Early detection can help alleviate the worsening side effects of acute withdrawal.
B. Withdrawal Syndrome (Acute Withdrawal)
The most intense withdrawal symptom appearance starts after a week of long-acting benzo. But for short-acting benzo users, physical symptoms start to diminish, but psychological remain constant or may aggravate during this phase.
This phase continues for another 10 to 14 days, and long-acting benzo withdrawal symptoms are at their peak.
C. Recurrence (Protracted Withdrawal)
Individuals who are heavy Benzo users or have been using them for a long time may experience post-acute withdrawal symptoms (PAWS). Recurrence usually takes place after a month of withdrawal treatment. They are sharp, random, and intense withdrawal symptoms such as persistent anxiety and insomnia. It is curable with the help of drug rehab experts.
Duration of Benzodiazepine Withdrawal
Benzodiazepines are characterized into three categories depending on their stay in the body
- Short-acting (Xanax and Halcion) 24-48 hours
- Intermediate-acting (Ativan and Restoril) 1-5 days
- Long-acting (Valium Librium®, Klonopin) 5-8 days
Benzo may stay differently in your body parts as such:
- Hair follicles can detect benzos for 4-6 months
- Urine for 1-7 days
- The blood stays lasts 12-24 hours
Whereas chronic misuse of benzos may stay in your body for up to 30 days.
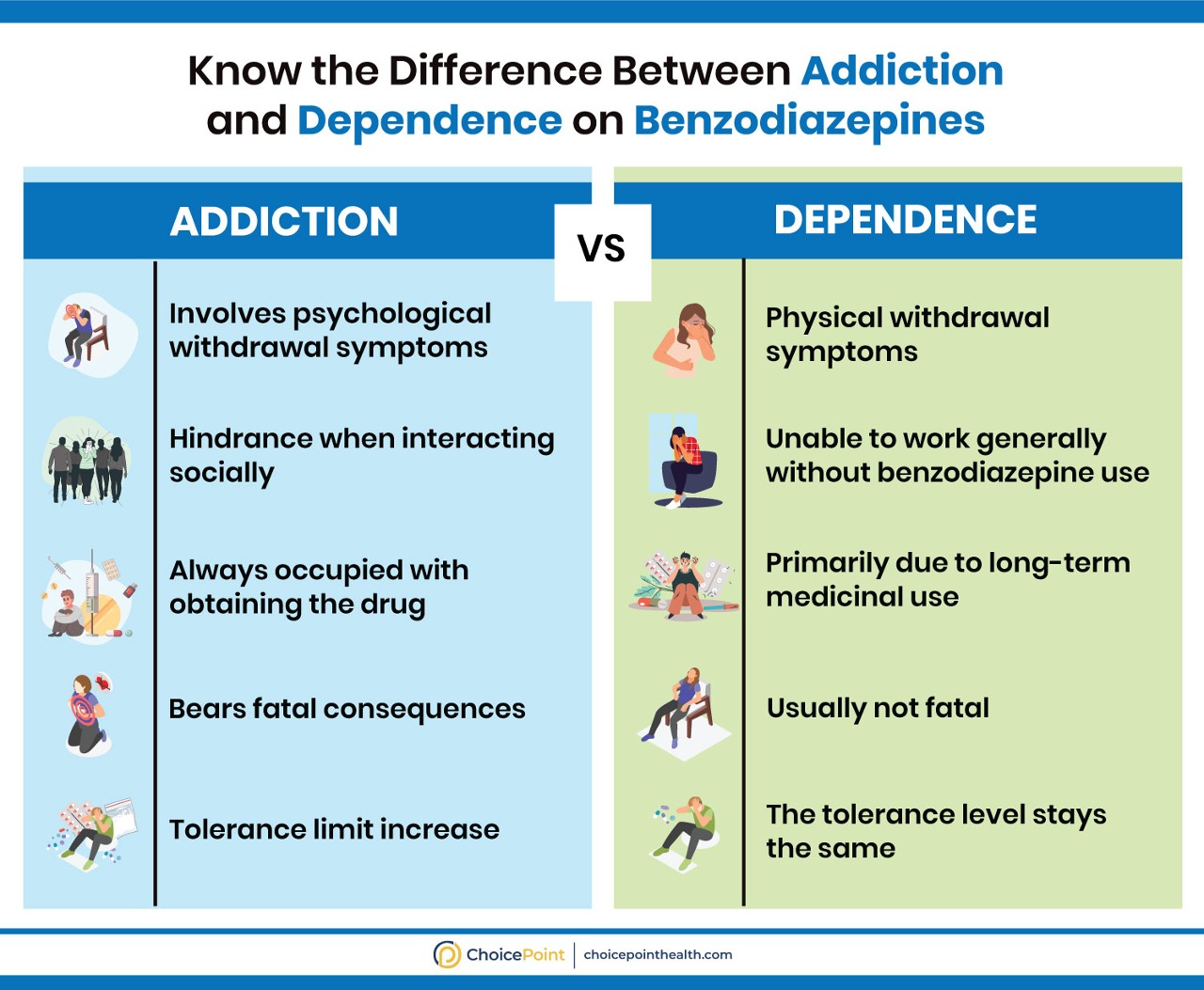
Benzodiazepines: Addiction and Dependence
Effective Protocols for Benzodiazepine Withdrawal Treatment
To stay safe from benzodiazepine side effects and its withdrawal when an individual quits, one should opt for inpatient drug rehab that provides structured care for benzo withdrawal treatment.
Benzodiazepine Detox: Medical Assistance to Withdrawal
Benzodiazepine withdrawal is specifically governed by medical detox that includes removing benzo toxication from the body while administering FDA-approved medications such as:
- Flumazenil antagonist to benzodiazepines
- Buspirone for treating anxiety disorders
- Buprenorphine such as Subutex for managing body pain and opioid withdrawal associated with benzo misuse
- Suboxone for opioid misuse, along with Benzos withdrawal
- Naltrexone for alcohol use disorder with benzodiazepine
It’s not a hard and fast rule to give only these medications, but practitioners may dispense others depending upon the severity and type of withdrawal symptoms associated with detox.
Covering BZD Psychological Withdrawal Symptoms With Psychotherapy
An estimated 30 million adults in the United States use benzos for mental health disorders, anxiety, and stress. To treat psychological symptoms and disorders associated with benzo withdrawal or co-morbidity, psychiatrists may dispense following psychotherapies.
- Cognitive Behavioral Therapy (CBT) to improve cognitive functioning by mending thinking behavior.
- Dialectical Behavior Therapy (DBT) to alleviate hyperactivity of the brain and excessive emotional imbalance.
Moreover, these therapies also help in preventing relapse and (PAWS) after one has completed the rehab process.
Supportive Care For Preventing Relapse Through Counseling
Personal development is the key to sober living. And benzodiazepines are the worst in destroying personal character as they affect the brain severely. For treating social withdrawal symptoms of benzos and building a sound character, psychiatrists may provide the following:
Social therapies, with one-on-one sessions, family members, and peer fellows at the inpatient rehab to give comprehensive care, share experiences, keep a record of relapses, and suggest behavioral changes to avoid stress factors.
ChoicePoint- Drug Rehab for Benzodiazepine Withdrawal Treatment
We know how it feels to be abandoned when you need the utmost care. ChoicePoint Drug Rehab offers exceptional services for treating benzodiazepine withdrawal with different levels of care:
- Inpatient
- High-Intensity outpatient/ Partial hospitalization
- Outpatient
- Telehealth
We offer commercial insurance programs, medicare, Tricare, and personal funding options for your treatment with individualized care, such as:
So verify your insurance to begin treatment the way you need! You can also try our free addiction assessment and discuss with us 844.445.2563.
Frequently Asked Questions Related to Benzodiazepine
People often get confused and struggle to quit Benzos, asking the following questions.
Can I Detox From Benzo Cold-Turkey?
“been through Benzo withdrawals, but it was Etizolam and went cold turkey; it was hell. I hope this is nothing like that, but I wonder if going cold turkey will be dangerous. I do have some valium as well.”
A Reddit user experiencing Benzo withdrawal symptoms
Quitting benzos suddenly. Comes with serious complications such as:
- Confusion
- Psychosis
- Seizures
Therefore, It is advised to gradually quit benzos with the help of inpatient drug rehab to avoid possible negative consequences!
Is Benzodiazepine Withdrawal Dangerous?
Benzo withdrawal is extremely uncomfortable and risky as it has higher chances of rebound symptoms and relapse. For people with co-occurring mental health conditions, it can prove fatal, and seizures occur. Therefore, it is advised to always opt for the highest level of care in the form of inpatient drug rehab to manage its detox.
How Long Can You Take Benzodiazepines?
Benzos should not take more than three weeks if you take it regularly. Exceeding this limit or increasing the dose may result in dependence and withdrawal symptoms.
How Benzodiazepine Withdrawal Affects the Brain?
Benzoddiapepine slows the brain by binding to GABA receptors that mainly decrease neuronal excitability during anxiety and stressful conditions. Thus repressing brain activity.
How Do I Get My Gaba Receptors Back to Normal?
You can adopt healthy habits such as:
- Meditation
- Yoga
- Swimming
- Nutritional therapy
- Taking vitamins
Inpatient rehab provides a structured aftercare plan to recover and maintain your GABA receptors, including all the above activities.
Can You Detox From Benzos at Home?
No! Benzodiazepine withdrawal is hazardous and comes with a lot of physical and psychological withdrawal symptoms that a person cannot manage on their own. Research suggests inpatient treatment in drug rehab is the best possible solution for comprehensive detox and preventing relapse.
Medical Disclaimer:
ChoicePoint aims to improve the quality of life for people struggling with substance use disorder and mental health issues. Our team of licensed medical professionals research, edit and review the content before publishing. However, this information is not intended to be a substitute for professional medical advice, diagnosis, or treatment. For medical advice please consult your physicians or ChoicePoint's qualified staff.










you are in reality a good webmaster The website loading velocity is amazing It sort of feels that youre doing any distinctive trick Also The contents are masterwork you have done a fantastic job in this topic